Smartwatch ECG vs Hospital ECG: How Accurate Is Wearable Heart Monitoring?
In the past, when we talked about an ECG (Electrocardiogram), we imagined hospital beds, multiple wires, and emergency rooms.
Today, ECG monitoring is on your wrist.
The real question is not whether wearable ECG technology works.
The question is how to use smartwatch ECG monitoring effectively for heart health, cardiovascular risk prevention, and long-term longevity.
This article explores how ECG on smartwatch devices works, how accurate it is, and what it means for people concerned about heart disease and stroke prevention.
What Is an ECG and How Is It Traditionally Performed in Hospitals?
An ECG (Electrocardiogram) measures the electrical signals that control your heartbeat.
The heart contracts rhythmically because of an internal electrical conduction system. The sinoatrial node (SA node) initiates electrical impulses, which can be recorded as waveforms.
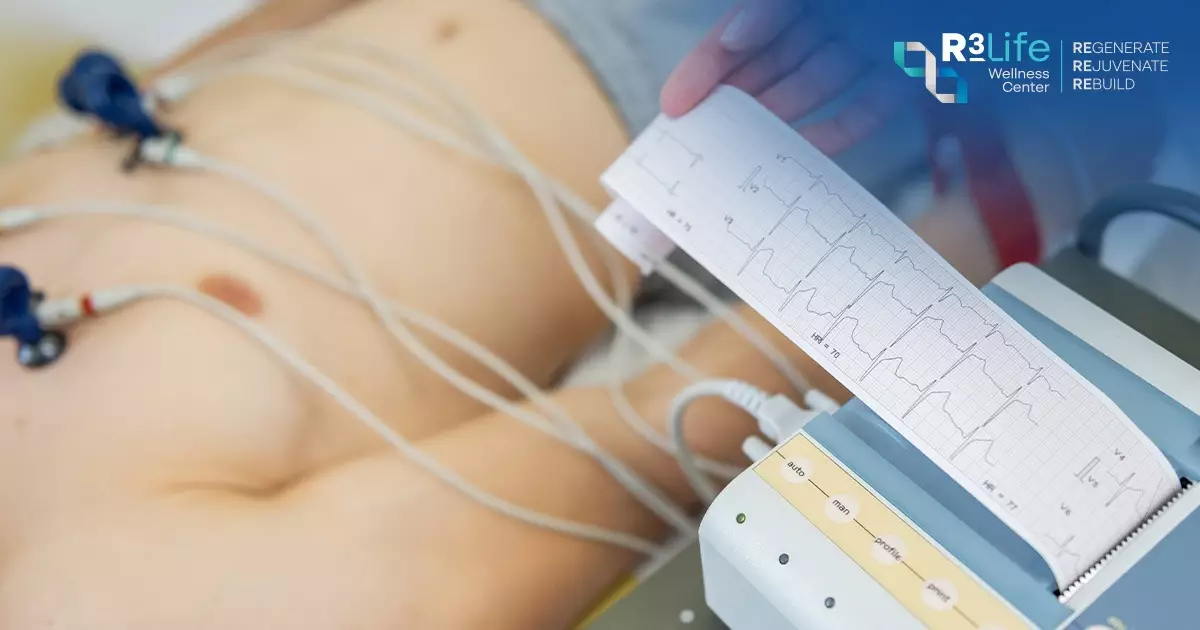
In hospitals, doctors perform a 12-lead ECG, attaching multiple electrodes to the chest, arms, and legs. This allows the heart to be evaluated from 12 different angles.
Physicians analyze components such as:
- P wave (atrial activation)
- QRS complex (ventricular contraction)
- T wave (ventricular recovery)
A hospital ECG is used to evaluate:
- Arrhythmia
- Myocardial ischemia
- Conduction abnormalities
Traditionally, ECG testing was performed when symptoms occurred, such as chest pain, palpitations, dizziness, or fainting.
How Can a Smartwatch Measure ECG?
Modern wearable devices use single-lead ECG technology.
The back of the smartwatch contains an electrode that touches the skin. When the user places a finger from the opposite hand on the digital crown or sensor, the device measures electrical potential differences similar to Lead I in a 12-lead ECG system.
This innovation is possible because of:
- Miniaturized biosensors
- Improved signal amplification
- AI-powered rhythm analysis
- Machine learning–based heart rhythm monitoring
In simple terms, the smartwatch does not diagnose disease independently. It compares your heart rhythm to large ECG pattern databases to detect irregularities.
Which Smartwatches Support ECG Monitoring?
Several wearable devices now offer ECG tracking functionality, including:
- Apple Watch Series 4 and newer
- WHOOP 5.0 (MG Sensor / Life package)
- Samsung Galaxy Watch Active 2, Watch 4, Watch 5, Watch 6 (region-dependent)
- Huawei Watch models
- Garmin Venu series (region-dependent)
ECG feature availability depends on regulatory approval in each country.
How Accurate Is Smartwatch ECG?
The Apple Heart Study published in the New England Journal of Medicine (2019), involving over 400,000 participants, demonstrated that smartwatch ECG could detect atrial fibrillation (AF) with high accuracy.
Multiple studies report sensitivity and specificity rates above 90% for AF screening using wearable ECG devices.
However, smartwatch ECG uses single-lead technology. It is highly useful for rhythm monitoring and early detection but does not replace a full 12-lead ECG for comprehensive cardiac diagnosis.
It should be viewed as an early-warning cardiovascular monitoring tool rather than a final diagnostic instrument.
Hospital 12-Lead ECG vs Smartwatch Single-Lead ECG
12-Lead ECG (Hospital-Based)
Electrodes are placed on multiple body locations, allowing multi-angle visualization of cardiac electrical activity. It provides comprehensive diagnostic information and is considered the clinical gold standard.
Single-Lead ECG (Smartwatch)
Measures electrical activity from one direction, primarily useful for rhythm monitoring such as detecting atrial fibrillation.
Neither is inherently superior in all contexts. They serve different purposes:
- Hospital ECG: Detailed diagnosis
- Smartwatch ECG: Daily rhythm monitoring and screening
What Can ECG Monitoring Help Detect?
Smartwatch ECG may help identify:
- Atrial Fibrillation (AF)
- Arrhythmia
- Tachycardia
- Bradycardia
Atrial fibrillation is associated with increased stroke risk. Early detection of irregular heart rhythm may allow earlier evaluation and preventive management.
However, ECG only reflects rhythm patterns. It does not measure cholesterol, vascular plaque, inflammation markers, or metabolic cardiovascular risk.

If You Are Concerned About Stroke or Heart Disease, What Should You Check?
Cardiovascular risk assessment goes beyond heart rhythm. Other important markers include:
- LDL-C and HDL-C
- Triglycerides
- Blood glucose
- Homocysteine (HCY)
Homocysteine is an amino acid associated with endothelial dysfunction and vascular inflammation. Elevated HCY levels have been linked in research to increased risk of stroke and coronary artery disease.
Notably, many annual health check-ups do not routinely include homocysteine testing.

Universe Health Check Up: A Broader Cardiovascular Risk Assessment Including HCY
Universe Health Check Up is an 18-parameter health screening program by R3 Life, designed as a more convenient alternative to a traditional annual hospital check-up.
The program includes 18 key markers, such as:
- Homocysteine (HCY) – vascular risk indicator
- Liver function (ALB, ALT, AST, GGT, etc.)
- Kidney function (Creatinine, Urea)
- Lipid profile (Triglycerides, HDL-C, LDL-C, Total Cholesterol)
- Blood glucose (GLU)
- Muscle inflammation marker (Total CK)
How Is It Different from a Standard Hospital Check-Up?
The key differences are speed, efficiency, and depth of analysis.
- Results are available within approximately 15 minutes.
- Only a small amount of blood is required.
- Most importantly, the program includes Homocysteine (HCY) testing, a crucial marker for assessing the risk of stroke and cardiovascular disease — a parameter that is often not included in standard annual hospital check-up packages.
Advanced Interpretation by ABAARM-Certified Physicians
Another significant difference of the Universe Health Check Up at R3 Life Wellness Center is that results are interpreted by physicians certified by the American Board of Anti-Aging and Regenerative Medicine (ABAARM).
Their approach differs from conventional hospital result interpretation.
Rather than simply determining whether results are “normal” or “abnormal,” anti-aging physicians analyze:
- Whether specific values indicate early trends or future disease risk
- Whether results fall within the normal range but are not optimal for your age, gender, or lifestyle
- The interrelationship between biomarkers, such as Homocysteine, lipid levels, inflammation, and vascular health
This means the check-up goes beyond reporting lab results. It extends into a personalized preventive strategy designed to reduce long-term cardiovascular risk before disease actually develops.
Universe Health Check Up is therefore not just about detecting disease — it is about gaining a deeper understanding of your health in order to design a personalized, proactive care plan tailored specifically to your body.
Know Your Risk. Then Act: HCY Lowering IV Drip
Elevated homocysteine typically causes no immediate symptoms. There is no smartwatch alert.
HCY Lowering IV Drip is designed as a preventive support strategy to help manage elevated homocysteine and support vascular health.
This approach is not an acute treatment but part of long-term cardiovascular risk management.
Cardiovascular disease develops gradually through years of microvascular damage. Prevention creates long-term difference.
Frequently Asked Questions about Smartwatch ECG
Q: Can a smartwatch ECG replace a hospital ECG?
A: No. A smartwatch uses single-lead technology, which is useful for rhythm monitoring and early detection of irregularities like atrial fibrillation. A full 12-lead hospital ECG remains the clinical gold standard for comprehensive cardiac diagnosis.
Q: How accurate is a smartwatch ECG for detecting atrial fibrillation?
A: Research, including the Apple Heart Study in the New England Journal of Medicine, has shown sensitivity and specificity above 90% for atrial fibrillation screening. It is a reliable early-warning tool but should not be treated as a final diagnostic instrument.
Q: If my smartwatch ECG looks normal, does that mean my heart is healthy?
A: Not necessarily. ECG only reflects rhythm patterns and does not measure cholesterol, blood glucose, inflammation, or homocysteine levels. A broader screening such as a Universe Health Check Up gives a more complete picture of cardiovascular risk.
Conclusion
ECG is no longer limited to hospitals. Smartwatch ECG monitoring has introduced accessible daily rhythm tracking with strong research support for atrial fibrillation screening.
Yet cardiovascular prevention extends beyond rhythm monitoring. Heart disease risk also involves inflammation, lipid imbalance, glucose metabolism, and homocysteine levels.
Technology is most powerful when used for prevention.
Monitoring risk is important. Acting on hidden risk factors is what protects long-term heart health.


 Longevity Monitoring: The Future of Health Beyond Annual Checkups
Longevity Monitoring: The Future of Health Beyond Annual Checkups





